Exploring Achilles Tendonitis
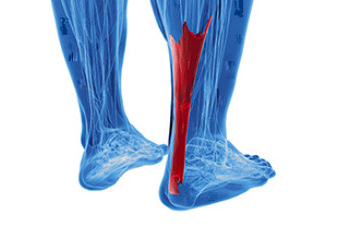
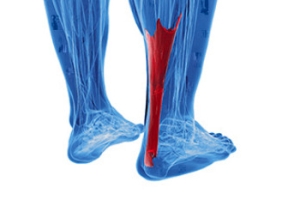
Achilles tendonitis is an ailment affecting the long tendon that connects the leg bones to the heel. This condition is particularly common among those engaged in high-impact activities, like running and jumping. The Achilles tendon's susceptibility to inflammation due to repetitive stress often leads to microtears and thickening. This results in Achilles tendonitis, which is characterized by posterior ankle pain and stiffness. However, the more severe consequence, an Achilles tendon rupture, typically occurs during forceful movements which result in sudden, intense pain and the inability to bear weight. Approximately 80 percent of Achilles tendon ruptures result in complete loss of function in the calf muscle. If you are experiencing pain in the Achilles tendon, it is suggested that you cease the activity causing the pain and make an appointment with a podiatrist as soon as possible. This foot doctor can conduct a thorough exam and determine the appropriate treatment.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact Jon McCreary, DPM of Fort Worth Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our office located in Fort Worth, TX . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Achilles Tendon Injuries
The Achilles tendon is the largest tendon in the body; it is a tough band of fibrous tissue that stretches from the bones of the heel to the calf muscles. This tendon is what allows us to stand on our toes while running, walking, or jumping, it is common for this tendon to become injured. In severe cases, the Achilles tendon may become partially torn or completely ruptured. However, this tendon is susceptible to injury because of its limited blood supply and the high level of tension it endures.
The people who are more likely to suffer from Achilles tendon injuries are athletes who partake in activities that require them to speed up, slow down, or pivot. Consequently, athletes who engage in running, gymnastics, dance, football, baseball, basketball, or tennis are more likely to suffer from Achilles tendon injuries. Additionally, there are other factors that may make you more prone to this injury. People who wear high heels, have flat feet, tight leg muscles or tendons, or take medicines called glucocorticoids are more likely to have Achilles tendon injuries.
A common symptom of an Achilles tendon injury is pain above the heel that is felt when you stand on your toes. However, if the tendon is ruptured, the pain will be severe, and the area may become swollen and stiff. Other symptoms may be reduced strength in the lower ankle or leg area, and reduced range of motion in the ankle. When the Achilles tendon tears, there is usually a popping sound that occurs along with it. People who have acute tears or ruptures may find walking and standing to be difficult.
If you suspect you have injured your Achilles tendon, you should see your podiatrist to have a physical examination. Your podiatrist will likely conduct a series of tests to diagnose your injury including a “calf-squeeze” test. Calf squeeze tests are performed by first squeezing the calf muscle on the healthy leg. This will pull on the tendon and consequently cause the foot to move. Afterward, the same test will be performed on the injured leg. If the tendon is torn, the foot won’t move because the calf muscle won’t be connected to the foot.
Various Types of Toenail Fungus
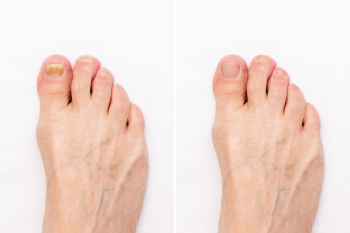
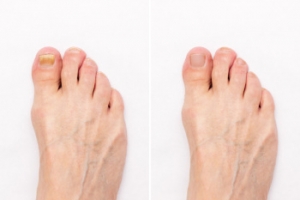
Toenail fungus, medically known as onychomycosis, encompasses several distinct types, each presenting unique characteristics and symptoms. The most common form is distal subungual onychomycosis, which typically begins as a yellow or white spot beneath the tip of the nail and gradually spreads deeper into the nail bed. Proximal subungual onychomycosis affects the base of the nail and is often seen in individuals with compromised immune systems. White superficial onychomycosis manifests as white spots on the surface of the nail, which can gradually expand. Candida onychomycosis is caused by yeast and can affect both fingernails and toenails, often leading to thick, discolored nails. Finally, total dystrophic onychomycosis results in complete nail destruction, characterized by thickening, discoloration, and crumbling of the nail plate. Recognizing the type of toenail fungus is essential for effective treatment. If you have toenail fungus, it is strongly suggested that you are under the care of a podiatrist who can accurately diagnose which type it is, and offer the treatment method that is right for you.
If left untreated, toenail fungus may spread to other toenails, skin, or even fingernails. If you suspect you have toenail fungus it is important to seek treatment right away. For more information about treatment, contact Jon McCreary, DPM of Fort Worth Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Symptoms
- Warped or oddly shaped nails
- Yellowish nails
- Loose/separated nail
- Buildup of bits and pieces of nail fragments under the nail
- Brittle, broken, thickened nail
Treatment
If self-care strategies and over-the-counter medications does not help your fungus, your podiatrist may give you a prescription drug instead. Even if you find relief from your toenail fungus symptoms, you may experience a repeat infection in the future.
Prevention
In order to prevent getting toenail fungus in the future, you should always make sure to wash your feet with soap and water. After washing, it is important to dry your feet thoroughly especially in between the toes. When trimming your toenails, be sure to trim straight across instead of in a rounded shape. It is crucial not to cover up discolored nails with nail polish because that will prevent your nail from being able to “breathe”.
In some cases, surgical procedure may be needed to remove the toenail fungus. Consult with your podiatrist about the best treatment options for your case of toenail fungus.
If you have any questions, please feel free to contact our office located in Fort Worth, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Treating Toenail Fungus
Fungal infection of the toenail, or onychomycosis, typically appears as a gradual change in a toenail’s texture and color that involves brittleness and darkening. The fungal infection itself occurs beneath the surface of the nail. Aside from discoloration, other symptoms include the collection of debris beneath the nail plate, white marks on the nail plate, and a foul odor emanating from the nail. If ignored, the infection can spread into other nails and the skin; in severe cases, it can hinder one’s ability to work or walk.
The toenails are particularly vulnerable to contracting infection in moist environments where people are likely to be walking barefoot, such as around swimming pools, public showers, and locker rooms. Fungal infection may also be more likely to occur in nail beds that have been injured, and sufferers of chronic diseases such as diabetes, circulatory problems, or immunodeficiency conditions are particularly prone to developing fungal nails.
Fungal nails can be primarily prevented by practicing proper hygiene and regularly examining the feet and toes. Carefully washing the feet with soap and water and thoroughly drying the feet afterwards are essential. Other tips include wearing shower shoes in public areas, changing shoes and socks daily, keeping toenails clipped at a short length, wearing breathable shoes that fit properly, wearing moisture-wicking socks, and disinfecting home pedicure tools and instruments used to cut nails.
Fungal nail treatment may vary between patients and the severity of the condition. Your podiatrist may suggest a daily routine of cleansing that spans over a period of time to ease mild infections. Over-the-counter or prescription antifungal agents may also be prescribed, including topical and/or oral medications. Debridement, or the removal of diseased nail matter and debris, may also be performed. In more severe cases, surgical treatment may be needed. In some instances, the temporary removal of the fungal nail allows for the direct application of a topical antifungal to the nail bed. In other cases, a chronically painful fungal nail that has not responded to other treatments may be permanently removed; this allows the infection to be cured and avoids the growth of a deformed nail.
Blistery Foot Woes

Blisters on the feet are often caused by friction from wearing ill-fitting shoes or engaging in prolonged physical activity. Corns can also result from burns, allergic reactions, or fungal infections. These fluid-filled pockets form as a protective response to pressure or irritation on the skin. While blisters are usually harmless, they can become painful if they rupture or get infected. Preventing blisters involves wearing properly fitting shoes, using moisture-wicking socks, and avoiding repetitive friction on the skin. Applying cushioning pads or bandages to high-friction areas can also help reduce the risk of blister formation. Podiatrists can provide treatment to relieve pain, prevent infection, and address underlying factors that contribute to blister formation, ensuring optimal foot health and comfort. If you have a foot blister that persists or has become painful or infected, it is suggested that you seek professional care from a podiatrist.
Blisters are prone to making everyday activities extremely uncomfortable. If your feet are hurting, contact Jon McCreary, DPM of Fort Worth Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters develop as a result of constantly wearing tight or ill-fitting footwear. This happens due to the constant rubbing from the shoe, which can often lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
How Do Blisters Form?
Blisters on the feet are often the result of constant friction of skin and material, usually by shoe rubbing. Walking in sandals, boots, or shoes that don’t fit properly for long periods of time can result in a blister. Having consistent foot moisture and humidity can easily lead to blister formation.
Prevention & Treatment
It is important to properly care for the affected area in order to prevent infection and ease the pain. Do not lance the blister and use a Band-Aid to provide pain relief. Also, be sure to keep your feet dry and wear proper fitting shoes. If you see blood or pus in a blister, seek assistance from a podiatrist.
If you have any questions, please feel free to contact our office located in Fort Worth, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Blisters
Blisters are pockets of fluid that occur under the top layer of your skin. These fluid pockets are usually filled with pus, blood, or serum. Blisters may itch or hurt and can appear as a single bubble or in clusters.
The most common types of blisters are friction blisters. This type of blister may be caused by wearing shoes that are too tight. Friction blisters can also occur on the hands. A change in temperature may also cause blisters on the feet. In the freezing air, frostbite on your toes can lead to blisters, as well as sunburn from hot weather.
The best way to treat a blister is to keep it clean and dry. Most blisters will get better on their own. Once the skin absorbs the fluid within the blister, it will flatten and eventually peel off. You should avoid popping your blister unless you podiatrist does it for you. Additional treatment options include applying an ice pack to the blister or using over-the-counter blister bandages to cover the affected area.
If your blister becomes discolored, inflamed, or worsens it is advised that you speak to your podiatrist. Blisters that are yellow, green, or purple may be infected and require immediate medical attention. Blisters that are abnormally colored may be a sign of a more serious underlying health condition such as herpes.
Managing Sore Feet

Your feet endure daily strain, often leading to soreness and discomfort. Home remedies like foot baths with Epsom salts, stretching exercises, and massages can offer temporary relief. In addition, strengthening routines, and wearing properly fitting footwear can help alleviate symptoms. However, if foot pain persists or worsens, or if you experience symptoms such as swelling, numbness, or difficulty walking, it may be time to consult a podiatrist. Individuals with diabetes should be particularly vigilant, as any foot pain or abnormalities may indicate serious complications that require immediate medical attention. Furthermore, if you have flu-like symptoms in combination with foot pain, an open wound in the foot, or suspect a broken bone, seeking help is essential. A podiatrist can accurately diagnose and treat underlying conditions, such as plantar fasciitis, neuropathy, or stress fractures. They also can provide personalized treatment plans, including custom orthotics for optimal support and alignment. By seeking timely professional help, you can address the root cause of your foot pain and prevent future discomfort. If your sore feet worsen, it is suggested that you schedule an appointment with a podiatrist for an exam.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Jon McCreary, DPM from Fort Worth Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact our office located in Fort Worth, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Foot Pain
The feet, being the foundation of the body, carry all of the body’s weight and are therefore prone to experiencing pain and discomfort. If you are experiencing foot pain, it is important to determine where in the foot you are experiencing this pain to help discover the cause of it. While pain can be experienced virtually anywhere in the foot, the most common sites of foot pain are in the heel and ankle.
Heel pain can be due to a multitude of conditions including plantar fasciitis, Achilles tendinitis, and heel spurs. Pain experienced in the ankle can be a sign of an ankle sprain, arthritis, gout, ankle instability, ankle fracture, or nerve compression. In more serious cases, pain in the foot can be a sign of improper alignment or an infection.
Foot pain can be accompanied by symptoms including redness, swelling, stiffness and warmth in the affected area. Whether the pain can be described as sharp or dull depends on the foot condition behind it. It is important to visit your local podiatrist if your foot pain and its accompanying symptoms persist and do not improve over time.
Depending on the location and condition of your foot pain, your podiatrist may prescribe certain treatments. These treatments can include but are not limited to prescription or over-the-counter drugs and medications, certain therapies, cortisone injections, or surgery.
If you are experiencing persistent foot pain, it is important to consult with your foot and ankle doctor to determine the cause and location. He or she will then prescribe the best treatment for you. While milder cases of foot pain may respond well to rest and at-home treatments, more serious cases may take some time to fully recover.
Foot and Ankle Stress Fractures in Athletes
Foot and ankle stress fractures encompass various types, commonly occurring among athletes due to repetitive impact activities like running, jumping, or sudden changes in direction. These fractures result from the accumulation of microtrauma, leading to small cracks in the bones. Athletes often describe the sensation as a gradual onset of localized pain that worsens with activity and improves with rest. Stress fractures can occur in different areas of the foot and ankle, including the metatarsals, navicular, calcaneus, and fibula. Prompt diagnosis is important to prevent further damage and facilitate proper healing. If you have sustained a foot or ankle injury, it is suggested that you schedule an appointment with a podiatrist. A podiatrist can employ techniques like imaging studies, biomechanical assessments, and customized treatment plans. By providing targeted interventions and guidance on activity modification, podiatrists help shorten your time away from sports and expedite your return to activity with reduced risk of complications.
Activities where too much pressure is put on the feet can cause stress fractures. To learn more, contact Jon McCreary, DPM from Fort Worth Podiatry. Our doctor can provide the care you need to keep your pain free and on your feet.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures occur in the foot and ankle when muscles in these areas weaken from too much or too little use. The feet and ankles then lose support when walking or running from the impact of the ground. Since there is no protection, the bones receive the full impact of each step. Stress on the feet can cause cracks to form in the bones, thus creating stress fractures.
What Are Stress Fractures?
Stress fractures occur frequently in individuals whose daily activities cause great impact on the feet and ankles. Stress factors are most common among:
- Runners
- People affected with Osteoporosis
- Tennis or basketball players
- Gymnasts
- High impact workouts
Symptoms
Pain from the fractures occur in the area of the fractures and can be constant or intermittent. It will often cause sharp or dull pain with swelling and tenderness. Engaging in any kind of activity which involves high impact will aggravate pain.
If you have any questions please feel free to contact our office located in Fort Worth, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.